Artroscopía para Desgarro o Ruptura de Meniscos de Rodilla
Puerto Vallarta – Riviera Nayarit
¡Devuélvele el movimiento a tu vida! – ¡Alivia el dolor, mejora la movilidad!
Sin listas de espera y con precios accesibles y competitivos

Dr. Max Greig - Cirujano Ortopedista Especialista en Cadera, Rodilla, Columna y Hombro
Con más de 25 años de Experiencia en Cirugia Ortopedica
Los desgarros de menisco se encuentran entre las lesiones de rodilla más comunes. Los atletas, particularmente aquellos que practican deportes de contacto, corren el riesgo de sufrir desgarros de menisco. Sin embargo, cualquier persona a cualquier edad puede romper el menisco. Cuando la gente habla de cartílago desgarrado en la rodilla, normalmente se refiere a un menisco desgarrado.
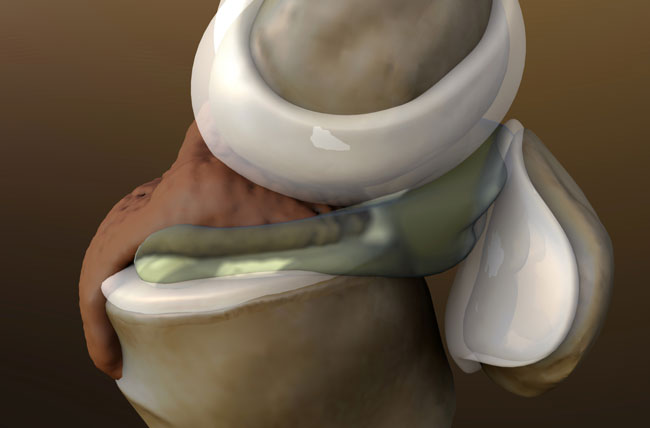
El menisco puede desgarrarse por un traumatismo agudo o como resultado de cambios degenerativos que ocurren con el tiempo. Las lágrimas se notan por su apariencia, así como por el lugar del menisco en el que se produce la rotura. Los desgarros comunes incluyen asa de cubo, solapa y radial.
Las lesiones de menisco relacionadas con los deportes a menudo ocurren junto con otras lesiones de rodilla, como los desgarros del ligamento cruzado anterior (LCA).
Sintomas
Es posible que sienta un chasquido al romper el menisco. La mayoría de las personas todavía pueden caminar con la rodilla lesionada y muchos atletas pueden seguir jugando con un desgarro. Sin embargo, al cabo de 2 o 3 días, la rodilla se irá poniendo gradualmente más rígida e hinchada. The most common symptoms of a meniscus tear are:
-
Dolor
-
Rigidez e hinchazón
-
Atrapamiento o bloqueo de la rodilla
-
La sensación de que tu rodilla cede
-
Incapacidad para mover la rodilla en todo su rango de movimiento.
Tratamiento Conservador o Cirugía
El tratamiento para un desgarro de menisco dependerá de su tamaño, de qué tipo es y de dónde se encuentra dentro del cartílago. Lo más probable es que su médico le recomiende descansar, usar analgésicos y aplicar hielo en la rodilla para reducir la hinchazón.
También pueden sugerir fisioterapia. Esto ayudará a fortalecer los músculos alrededor de la rodilla y a mantenerla estable.
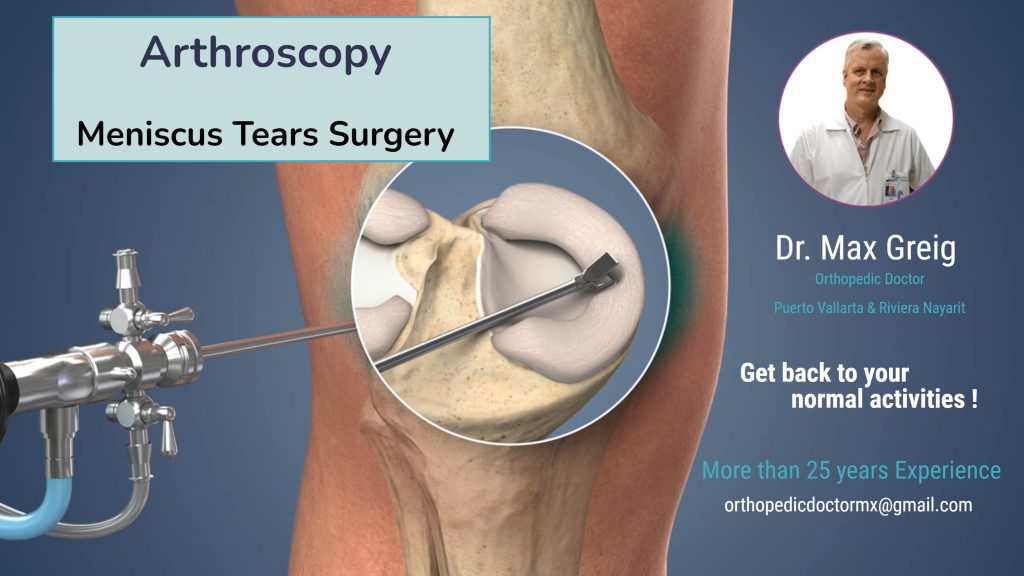
Si estos tratamientos no funcionan, o si su lesión es grave, es posible que le recomienden una cirugía. Dr. Greig le solicitará una resonancia magnética y es posible que observe el desgarro con un artroscopio. Es una herramienta delgada que tiene una cámara y una luz al final. Permite a los médicos ver el interior de las articulaciones. Si el examen muestra que su desgarro de menisco es leve (Grado 1 o 2), es posible que no necesite cirugía. Si es grado 3, probablemente lo harás. Su médico podría optar por realizar cualquiera de las siguientes opciones:
Reparación artroscópica.-Dr. Greig hará pequeños cortes en su rodilla. Insertarán un artroscopio para observar bien el desgarro. Luego colocarán pequeños dispositivos que parecen dardos a lo largo del desgarro para coserlo. Su cuerpo los absorberá con el tiempo.
Meniscectomía parcial artroscópica.- Se extraerá un trozo del menisco desgarrado para que su rodilla pueda funcionar normalmente.
Meniscectomía total artroscópica. Durante este procedimiento, su médico extirpará todo el menisco.
La reparación de menisco es de bajo riesgo. Las complicaciones son raras. Pueden incluir lesiones a los nervios de la piel, infecciones y rigidez de las rodillas. Su médico puede recetarle antibióticos para ayudar a prevenir la infección. También pueden recomendar medias de compresión para ayudar a prevenir coágulos de sangre.
¿Por qué los pacientes norteamericanos prefieren Puerto Vallarta para recibir asistencia médica?

Puerto Vallarta y Riviera Nayarit en la Bahía de Banderas, México, son uno de los destinos turísticos más populares del mundo, con más visitantes cada año en busca de una hermosa ciudad para recibir tratamientos médicos, ahorrar dinero y ser atendido por los médicos más experimentados de México.
Encontrará médicos especialistas con experiencia y hospitales altamente calificados que ofrecen al turista que busca atención médica, atención y servicio de clase mundial, con infraestructura y tecnología médica de punta, para ofrecer diagnóstico, intervención, rehabilitación y recuperación.
- -Calidad Clínica y Médica
- Infraestructura Clínica de vanguardia
- *Atención Personalizada.-Altos estándares de capital humano calificado.
- Precios accesibles . Ahorro de costo hasta un 60 %. en comparación de los precios en Norteamérica
- -Los tiempos de espera son inexistentes. Realice su cirugía y planifíquela con una o dos semanas de anticipación. Vuelve pronto a tus actividades normales
- -Tiempo de viaje. Oportunidad de recuperarse en un hermoso y seguro destino de playa.
- Afinidad cultural. Las personas más amables de México
- *-Geografía. Debido a su ubicación, México es la opción perfecta para pacientes que viajan desde América del Norte, EE. UU. y Canadá y América del Sur.

Esta usted considerando Cirugia de Artroscopia ?
¡Permítanos guiarle a través del proceso con cuidado personal, profesionalismo y experiencia!
Mande un email:
orthopedicdoctormx@gmail.com
Para tener una comunicación más fácil con el especialista por favor proporcione la siguiente información:
Copias de los informes médicos más recientes.
Copias de imágenes (rayos X, tomografías computarizadas, ecografías y/o resonancias magnéticas, etc.)
Una pequeña narración del paciente contando su historia y síntomas que ayuda al especialista a comprender las condiciones del paciente.
Imágenes de la zona afectada.
(Para visitantes al destino) Posibles fechas en las que puedes viajar a Puerto Vallarta o Riviera Nayarit
Nombre completo del paciente
NUM. TELÉFONO (10 Dígitos)
CMQ Hospital Riviera Nayarit
Av. Héroes de Nacozari 280 Bucerías, 63732 Riviera Nayarit, Nay.
orthopedicdoctormx@gmail.com

